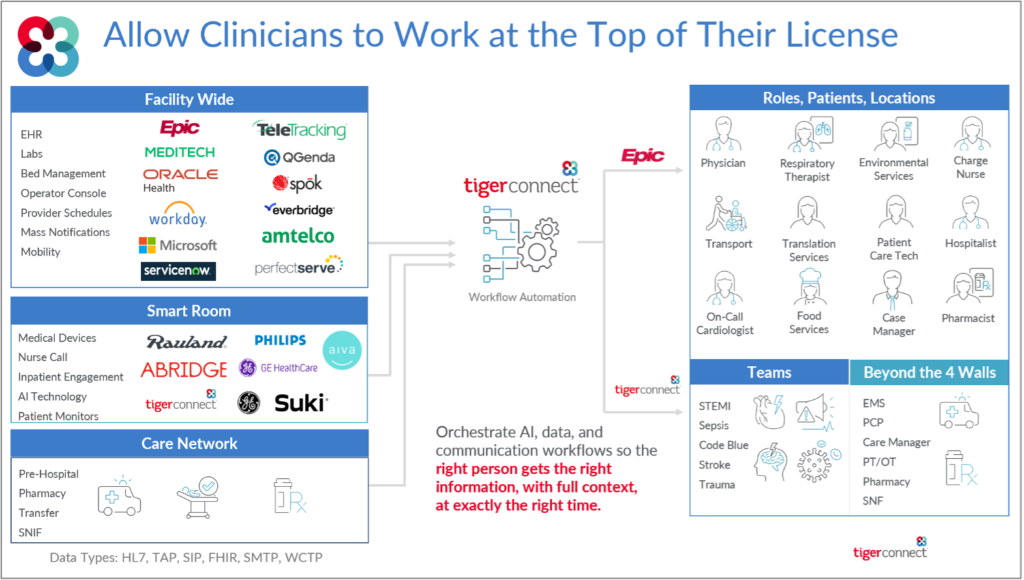
Better orchestration of care team workflows drives better clinical outcomes, higher efficiency, and meaningful financial returns. In an environment where operational performance is a primary axis of competition among health systems, how work moves through the organization increasingly determines how well the organization performs. Communication orchestration—when treated as a strategic capability rather than a collection of tools—can materially move the bottom line.
A growing body of evidence supports this claim.
The Evidence: Where Orchestration Delivers ROI
1. Throughput and Revenue
In perioperative and Operating Room environments, improved orchestration of teams, rooms, and resources leads to higher throughput and increased revenue. More reliable on-time starts, faster room turnover, and reduced idle capacity directly translate into financial gains for hospitals operating at or near capacity [1].
2. Operational Efficiency
In clinic settings, orchestration of workflows has been shown to reduce:
- Total cycle times by 21%
- Patient wait times by 64%
- Facility costs by an average of $39 per consult visit
In one multi-site study, these improvements resulted in approximately $5 million per year in cumulative savings for the participating health system [2, 3].
3. Patient and Staff Satisfaction
Patient satisfaction improves when care delivery is more predictable, coordinated, and transparent. Studies of Lean methodologies, supported by digital communication and workflow tools, demonstrate improvements not only in patient experience but also in staff engagement and perceived teamwork [4, 5].
4. Quality and Clinical Outcomes
Orchestration also impacts quality and safety:
- Inpatient rapid response team orchestration has been associated with reduced length of stay (LOS), lower mortality, and a 23% reduction in hospital expenditures [6, 7].
- Time-sensitive care pathways—such as Door-to-Diagnosis and Door-to-Treatment workflows—improve outcomes while reducing LOS when communication and task activation are precisely coordinated [8].
5. Total Cost of Ownership (TCO)
Finally, there is a compelling economic argument for simplifying the healthcare communication technology stack. Moving from a fragmented “toolbox” of point solutions to a platform-based approach through application rationalization (AppRat) can reduce total cost of ownership (TCO) by 20–30%. These savings come from:
- Improved clinical workflow efficiency
- Reduced licensing and vendor management costs
- Lower support and training burden
- Labor savings
- Reduced cybersecurity risk
Collectively, these factors materially improve enterprise economics [9].
Hard ROI and Soft ROI—Both Matter
Taken together, these data demonstrate improvements in both Hard ROI (revenue growth, cost reduction, asset utilization), and Soft ROI (patient experience, staff satisfaction, organizational reliability).
At TigerConnect, we have consistently observed that large health systems often operate with 50 or more point solutions in the communication space alone. This technology sprawl creates operational friction, support complexity, and a significant cognitive burden for clinicians.
The healthcare communication market is ripe for disruption through platform thinking. Health systems that get this right will successfully differentiate themselves both operationally and competitively. Highly reliable organizations require highly reliable core platforms. Period.
Lessons from the Front Lines
I have seen the benefits of addressing these challenges firsthand, both as a hospitalist and as a Chief Health Information Officer.
“Discharge Ready” programs are a practical example. Orchestrated interdisciplinary huddles—supported by coordinated messaging and digital status boards—help move med-surg patients to discharge earlier in the day. The result is fewer avoidable bed-days per year, lower costs, and improved capacity for new admissions.
In a prior organization, we applied similar principles in a ‘smart’ building dedicated to same-day surgery. The building itself was “wired” to support orchestration: measuring discharge readiness, optimizing throughput, and even tracking post-operative ambulation using remote tracking and location services as part of an automated discharge checklist. These capabilities allow us to make data-driven adjustments to workflows in near real time.
So, what can we do?
Elevating Communication Orchestration to a Strategic Pillar
Healthcare Communication Orchestration should be treated as a core strategic pillar. At TigerConnect, we view it as one of four foundational pillars of health system digital infrastructure:
- Clinical Applications: EHRs and related systems serving as the system of record.
- Data Infrastructure: Cloud compute and storage, data warehouses, and analytics platforms.
- Business Applications: Enterprise systems that run the organization, including ERP and revenue cycle platforms.
- Healthcare Communication Orchestration (Emerging but Critical): A historically fragmented space composed of systems that do not coordinate with one another, placing clinicians in the untenable role of acting as “middleware.”:
- Single-purpose communication tools
- Fleets of mobile devices
- Disconnected biomedical devices generating millions of alerts and alarms
The good news is that this fragmentation can be addressed today and while health systems have historically focused on pillars 1, 2, and 3, they are now recognizing that rationalizing and orchestrating this domain improves performance across all ROI dimensions—including care quality and safety.
Making It Real: The Smart(er) Hospital Scenario
Consider a health system planning a new hospital tower opening in three to four years. Floor plans are finalized. Infrastructure is specified. The goal is clear: a “smart” building—ideally smarter than the competitor down the road. The EHR is selected. Consultants are engaged.
But critical questions remain: How will this advanced technology fundamentally change the way we work? How will it help us be the very best? How will it enable us to explore new, innovative things? How will we be highly reliable, situationally aware, agile, and future-proofed? How will it return value?
The answer lies in planning for precise orchestration of teams through automated workflows, where the building and the rooms within it become active participants in care delivery.
Based on the evidence reviewed above, failure to plan for automated workflow orchestration and precision communication represents a 20–30% opportunity cost risk for any major digital healthcare investment.
What “Good” Can Look Like
In a realistic future-state scenario:
- Smart hospitals and smart rooms interact with Ambient AI and AI agents through orchestrated workflows.
- An orchestration engine detects events, activates teams, and coordinates tasks automatically.
- Real-time data identifies bottlenecks and recommends “next best actions.”
- Situational awareness across the enterprise increases exponentially.
- Patient flow through the ORs, procedural suites, and ChemoRx chairs is optimized with anticipatory load-balancing and high rates of on-time starts.
- Surgeons trust and respond to “room ready” notifications, and cart preferences are optimized.
- Patients get well in a supportive and patient-centered environment.
- Technology recedes into the background, allowing clinicians to focus on caring—not coordination. Restoring joy, meaning, and purpose to the profession.
Wasted capacity is reduced or eliminated, throughput is maximized, and health systems can realize 5–10× ROI from digital investments in communication orchestration.
Looking Ahead
In the next installment of this series, I will explore how AI—when applied thoughtfully within Healthcare Communication Orchestration—can further accelerate performance and differentiate health systems in an increasingly competitive landscape.
- https://pubmed.ncbi.nlm.nih.gov/30629927/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC9745696/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC11225068/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC7792026/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC8990690/
- https://pubmed.ncbi.nlm.nih.gov/25070310/
- https://pmc.ncbi.nlm.nih.gov/articles/PMC12036571/
- https://pubmed.ncbi.nlm.nih.gov/26828644/
- https://healthsystemcio.com/2025/12/01/application-rationalization-critical-complex-and-absolutely-attainable/
Featured Resources
Related Articles